Estimated reading time: 8 minutes
Key Takeaways
- Pancreatic cancer typically results from multiple factors rather than a single cause
- Age and smoking are the most significant risk factors
- About 10% of cases are hereditary, linked to inherited genetic mutations
- Environmental exposures play a minor role for most people
- Risk reduction is possible through lifestyle modifications like quitting smoking and maintaining healthy weight
Table of contents
Introduction
A diagnosis of pancreatic cancer naturally leads to urgent questions about its origins. Patients and families seek to understand why this disease develops, searching for clarity amid a complex landscape of medical information.
This guide explains the known contributors to pancreatic cancer, distinguishing between factors that increase risk and specific genetic causes. It synthesizes current evidence from leading sources like the Mayo Clinic and the American Cancer Society into a clear, compassionate resource for those seeking answers and a path forward.
The Current Understanding of Pancreatic Cancer Causes
Medical science has not identified a single, universal cause for pancreatic cancer. Instead, the disease typically emerges from a confluence of factors.
Key points frame our current knowledge:
- Multiple contributors are the rule. Pancreatic cancer usually results from several risk factors acting together over time, not one isolated trigger.
- Age is a primary factor. The vast majority of diagnoses occur in individuals over 65.
- Genetics and environment both play roles. A combination of inherited susceptibility, lifestyle choices, and sometimes environmental exposures sets the stage.
- Inherited mutations account for a subset. Approximately 10% of cases are linked to specific genetic mutations passed through families.
- Some risks are within our control. While we cannot change age or genetics, modifying behaviors like smoking and diet can meaningfully lower risk.
This multifaceted view is supported by ongoing research from major cancer institutions.
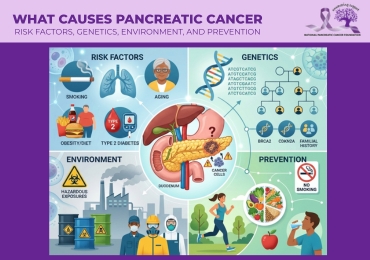
Pancreatic Cancer Risk Factors: A Closer Look
A risk factor increases the statistical likelihood of developing a disease. It is not a definitive cause, and many people with several risk factors never develop pancreatic cancer, while others with few known risks do.
You can read more about the range of known risk factors and how they are studied through comprehensive research.
Non-Modifiable Risk Factors
Age: Risk rises significantly after age 60, with most patients diagnosed between 65 and 80.
Sex and Race: Men face a slightly higher risk than women. Black individuals have a higher incidence than white, Asian, or Hispanic individuals, and people of Ashkenazi Jewish descent also have elevated risk, pointing to complex socioeconomic and genetic influences.
Family History: Having one or more first-degree relatives (parent, sibling, child) with pancreatic cancer increases personal risk. This often signals an underlying genetic component.
Potentially Modifiable Risk Factors
Tobacco Use: Smoking is the most significant modifiable risk factor, doubling the risk and contributing to an estimated 20-30% of cases. The risk declines gradually after quitting.
Obesity and Physical Inactivity: A body mass index (BMI) over 30 is associated with about a 20% higher risk. Abdominal fat and sedentary habits appear particularly influential.
Chronic Conditions: Long-standing type 2 diabetes increases risk, while new-onset diabetes after age 50 can sometimes be an early symptom of the disease. Chronic pancreatitis, often linked to heavy alcohol use, substantially elevates risk. Learn more about pancreatitis and how it differs from pancreatic cancer.
Diet: Some studies suggest diets high in red and processed meats may increase risk, while diets rich in fruits and vegetables may be protective.
Taken together, established risk factors explain roughly 40% of pancreatic cancer cases. The remainder arise from unknown or poorly understood interactions, highlighting the need for continued research.
The Role of Inherited Genetics
Inherited genetic mutations are present from birth in every cell. They account for about 10% of pancreatic cancers and define hereditary cancer syndromes.
Key genes implicated include:
- BRCA1 and BRCA2: Known for breast and ovarian cancer risk, these genes also increase pancreatic cancer susceptibility, particularly BRCA2.
- PALB2: A partner gene to BRCA2, with similar implications.
- ATM, CDKN2A, MLH1/MSH2 (Lynch syndrome), and STK11 (Peutz-Jeghers syndrome): Mutations in these genes are associated with specific syndromes that include elevated pancreatic cancer risk.
Genetic counseling is recommended for individuals with a strong family history, such as multiple close relatives with pancreatic cancer, early-onset diagnoses, or known family mutations. A counselor can assess risk, guide testing decisions, and help interpret results for the entire family.
Environmental and Occupational Exposures
The term “environmental toxins” encompasses chemicals and pollutants encountered in some workplaces or communities. Evidence linking them to pancreatic cancer is less robust than for factors like smoking.
The strongest data points to occupational settings. Workers with long-term, high-level exposure to certain pesticides, dyes, chemicals used in metal refining, and petrochemicals may face a modestly increased risk. Read more about occupational exposure risks.
For the general public, everyday environmental pollution is considered a minor contributor compared to lifestyle factors. Those with occupational exposures should follow safety protocols meticulously and discuss their history with a healthcare provider.
The Interaction of Multiple Factors
Pancreatic cancer is best understood as a multifactorial disease. A person’s individual risk profile is built from layers of influence.
Consider this scenario: A person may inherit a BRCA2 mutation, creating a genetic predisposition. If that person also smokes for decades, the risk compounds. Later, a diagnosis of type 2 diabetes adds another layer. No single factor is the sole cause; rather, the interaction between genetics and lifestyle over a lifetime culminates in disease development.
This complexity is why personalized risk assessment, which weighs all contributing elements, is more informative than focusing on any one factor in isolation.
Practical Steps for Risk Management and Support
While some risks cannot be altered, proactive management of others offers a tangible path to risk reduction.
You can find practical prevention strategies and lifestyle guidance for reducing your risk.
For the General Public:
- Avoid tobacco in any form. This is the most impactful preventive step.
- Maintain a healthy weight. Aim for a balanced diet and at least 150 minutes of moderate exercise per week.
- Limit alcohol consumption to reduce the risk of chronic pancreatitis.
- Be aware of symptoms, such as new jaundice (yellowing skin/eyes), unexplained weight loss, persistent abdominal pain, or new-onset diabetes after age 50, and seek prompt medical evaluation.
For Those with Increased Risk (Family History or Known Syndrome):
- Seek genetic counseling to understand your personal and familial risk landscape.
- Discuss screening options with a specialist. High-risk individuals may be candidates for surveillance with MRI or endoscopic ultrasound, though this is not recommended for the general population. See detailed screening guidance.
- Be vigilant about modifiable factors. For those with genetic susceptibility, maintaining a healthy lifestyle is especially critical.
For Patients and Families:
- Connect with support organizations for medical information, caregiver resources, and emotional support.
- For patients, genetic testing may identify mutations that qualify them for targeted therapies.
- Families can benefit from shared information and mutual support when navigating risk, screening, and care.
Frequently Asked Questions
Is pancreatic cancer hereditary?
About 10% of cases are considered hereditary, driven by inherited mutations. A strong family pattern of pancreatic, breast, ovarian, or colorectal cancer may indicate a hereditary syndrome.
Can pancreatic cancer be prevented?
There is no guaranteed prevention, but risk can be significantly reduced by not smoking, maintaining a healthy weight, exercising, and managing conditions like diabetes.
Do environmental chemicals cause pancreatic cancer?
For most people, general environmental exposure plays a very small role. Higher-risk exposures are typically long-term and occupational, such as in certain agricultural or industrial settings. More on occupational risks.
Should I get genetic testing?
Testing may be appropriate if you have multiple close relatives with pancreatic cancer, a relative diagnosed at a young age, or a known family mutation. A genetic counselor can help you make this decision.
If I have a high-risk job, what should I do?
Use all recommended personal protective equipment, adhere to workplace safety standards, and document your exposure history. Share this history with your doctor for informed health monitoring.
For Support and Information:
- The National Pancreatic Cancer Foundation (NPCF) offers helplines, support groups, and educational materials for patients and families. Find NPCF resources.
- The National Cancer Institute provides comprehensive information on cancer genetics.
- The American Cancer Society details guidelines for cancer prevention and healthy living.
Taking Action:
- If concerned about family history, speak with your doctor about a referral for genetic counseling.
- Integrate healthy lifestyle choices as consistent, long-term habits.
- Share this information with family members to promote collective awareness.
- Consider supporting organizations dedicated to pancreatic cancer research and patient support.
Understanding the causes of pancreatic cancer empowers informed decisions about health and risk management. You are not alone in seeking these answers; professional guidance and supportive communities are available to help.
This content is for educational purposes and is not a substitute for professional medical advice. Always consult your healthcare provider for personal health concerns.